Beyond the Armor: A Clinical Guide to Harlequin Ichthyosis in the Newborn
Navigating the physiological challenges, genetic foundations, and intensive care strategies for infants born with the rarest of skin conditions in .
The Clinical Landscape of Harlequin Ichthyosis
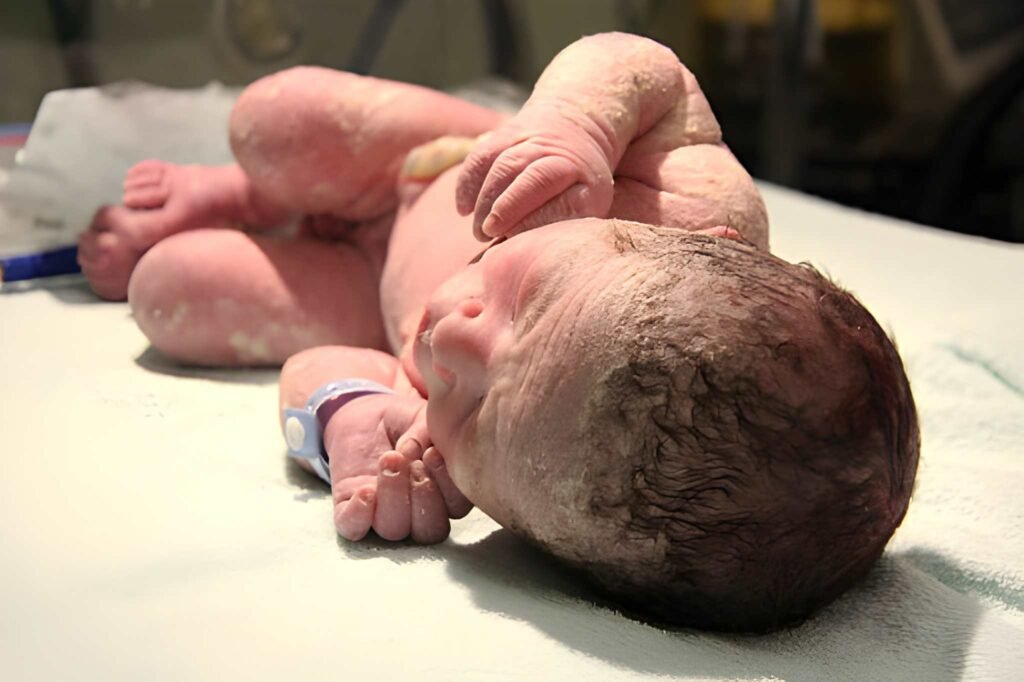
Harlequin Ichthyosis (HI) represents the most severe and rare manifestation of autosomal recessive congenital ichthyosis. At the moment of birth, the infant presents a striking and often distressing clinical picture, characterized by thick, plate-like scales that encase the entire body. These plates, separated by deep red fissures, create a biological armor that compromises every primary function of the skin, including barrier protection, thermoregulation, and moisture retention.
In the United States, the incidence remains exceptionally low, occurring in approximately 1 out of every 300,000 live births. Historically, the medical community viewed this condition as universally fatal within the first few days of life due to sepsis or respiratory failure. However, advancements in neonatal intensive care and the introduction of systemic retinoid therapy have radically shifted the prognosis. Today, infants born with Harlequin Ichthyosis not only survive the neonatal period but can transition into a managed, albeit intensive, lifelong dermatological routine.
Harlequin Ichthyosis is among the rarest genetic disorders documented in modern neonatology.
The ABCA12 Genetic Blueprint
The etiology of Harlequin Ichthyosis resides in a profound genetic failure within the ABCA12 gene. This gene provides the instructions for producing a protein essential for the transport of lipids (fats) in the cells that make up the outermost layer of the skin. Under normal conditions, these lipids are transported into the extracellular space to form a mortar-like barrier between skin cells. This barrier prevents water loss and blocks environmental pathogens.
In a newborn with Harlequin Ichthyosis, the mutation leads to a complete absence or severe dysfunction of the ABCA12 protein. Consequently, the lipid barrier fails to form. The skin compensates for this lack of barrier by producing massive amounts of keratin, leading to the hyperkeratosis that defines the condition. This process starts early in the second trimester, meaning the infant is already encased in thick scales while in the womb.
Harlequin Ichthyosis follows an autosomal recessive inheritance pattern. If both parents are asymptomatic carriers of the ABCA12 mutation, the following statistical outcomes apply to each pregnancy:
Probability of an Affected Child: 25%Probability of a Carrier Child: 50%
Probability of a Non-Carrier Child: 25%
Equation: 1/4 (Affected) + 1/2 (Carrier) + 1/4 (Normal) = 1.0 (Total Probability)
Anatomy of the Newborn Armor
The physical appearance of the Harlequin neonate is characterized by large, diamond-shaped scales. These scales exert mechanical pressure on the developing features of the infant, leading to several specific anatomical distortions that require immediate clinical attention.
| Anatomical Marker | Clinical Description | Primary Clinical Risk |
|---|---|---|
| Ectropion | The pulling back of the eyelids, exposing the conjunctiva. | Severe corneal drying and ulceration. |
| Eclabium | The outward turning of the lips, creating a fixed, open mouth. | Dehydration and feeding difficulties. |
| Restricted Thorax | Constriction of the chest wall by thick, rigid scales. | Respiratory distress and hypoventilation. |
| Digital Ischemia | Scale bands around fingers and toes (pseudo-ainhum). | Auto-amputation or loss of blood flow to limbs. |
Beyond these markers, the infant often has rudimentary or hidden ears due to the thickness of the keratin plates. The nostrils may be obstructed, forcing the newborn to breathe solely through the mouth. The clinical team must prioritize these areas during the first few minutes of life to ensure a patent airway and protection of the ocular surfaces.
Acute NICU Stabilization
Stabilization of a newborn with Harlequin Ichthyosis requires a multidisciplinary approach involving neonatologists, dermatologists, and specialized nursing staff. The primary goals in the first 48 hours focus on fluid management, temperature regulation, and antimicrobial protection.
The infant must reside in a high-humidity isolette (often 80% to 90% humidity) to prevent transepidermal water loss. High humidity also helps soften the keratin plates, facilitating natural shedding.
Because the skin barrier is non-functional, water loss occurs at a rate 5 to 10 times higher than in a term infant. Intravenous fluids must be calculated carefully to prevent electrolyte imbalances.
Temperature regulation remains exceptionally difficult. The thick scales act as an insulator, preventing the dissipation of heat, while the fissures allow heat to escape rapidly. This leads to profound thermal instability. The NICU team must utilize skin probes placed on the few available areas of soft skin to monitor the core temperature precisely.
Dermatological Protocols and Retinoid Therapy
The hallmark of modern treatment is the early administration of oral retinoids, such as Acitretin or Isotretinion. These medications accelerate the shedding of the thick keratin plates and normalize the growth of new skin cells. When initiated within the first few days of life, retinoid therapy significantly reduces the duration of the "armor" phase and improves the flexibility of the chest wall.
The deep fissures between the scales are the primary entry points for bacteria (commonly Staphylococcus aureus). Treatment involves the application of topical antibiotics and silver-based dressings. Nurses must perform meticulous skin checks every 2 to 4 hours to identify new areas of breakdown.
Aggressive lubrication of the eyes with thick ointments is mandatory every hour to prevent corneal scarring. Ears must be cleaned of keratin debris to prevent the development of a permanent hearing loss caused by physical obstruction of the ear canal.
The mechanical pulling of the scales and the exposure of raw skin in the fissures is profoundly painful. Newborns require scheduled analgesia (often including low-dose opioids or acetaminophen) to allow for movement and physical therapy, which prevents joint contractures.
Survival and Multidisciplinary Life
Surviving the neonatal period is just the beginning of the journey. Children with Harlequin Ichthyosis require 3 to 4 hours of skin care every single day for the rest of their lives. This includes long baths to hydrate the skin, followed by the application of heavy emollients. While the "armor" does not return, the skin continues to grow at a rate 5 to 10 times faster than normal, leading to constant peeling and redness.
Nutrition also becomes a lifelong challenge. Because the body is constantly "growing a new skin," the caloric requirements of these children are significantly higher than their peers. Many children with HI require a high-calorie diet supplemented with protein to maintain a normal growth curve. Without this, they often experience "failure to thrive" due to the massive metabolic demand of hyperkeratosis.
The Parental Journey
For the parents of a newborn with Harlequin Ichthyosis, the experience is often one of profound shock and grief. The visual difference of their child, combined with the intensity of the medical interventions, can lead to a sense of isolation. Support groups and connections with other families living with ichthyosis are vital components of the care plan.
It is important for the medical team to encourage bonding as early as possible. Once the infant is stable, skin-to-skin contact (while using appropriate barrier protections) helps establish the parent-child bond. Parents must be trained early in the complex skin-care routines, as they will eventually become the primary "specialists" in their child's daily care. With the right support, these children grow to have successful social lives, education, and careers, proving that life beyond the armor is not only possible but can be exceptionally vibrant.
In summary, Harlequin Ichthyosis in the newborn is a clinical emergency that demands an immediate, coordinated, and aggressive response. By focusing on the ABCA12 genetic failure and its physiological consequences—dehydration, infection, and respiratory restriction—the medical team can bridge the gap from birth to stability. The introduction of oral retinoids has turned what was once a terminal diagnosis into a manageable chronic condition. While the journey remains arduous, the resilience of these infants and the dedication of their families remain a testament to the power of modern neonatal science.