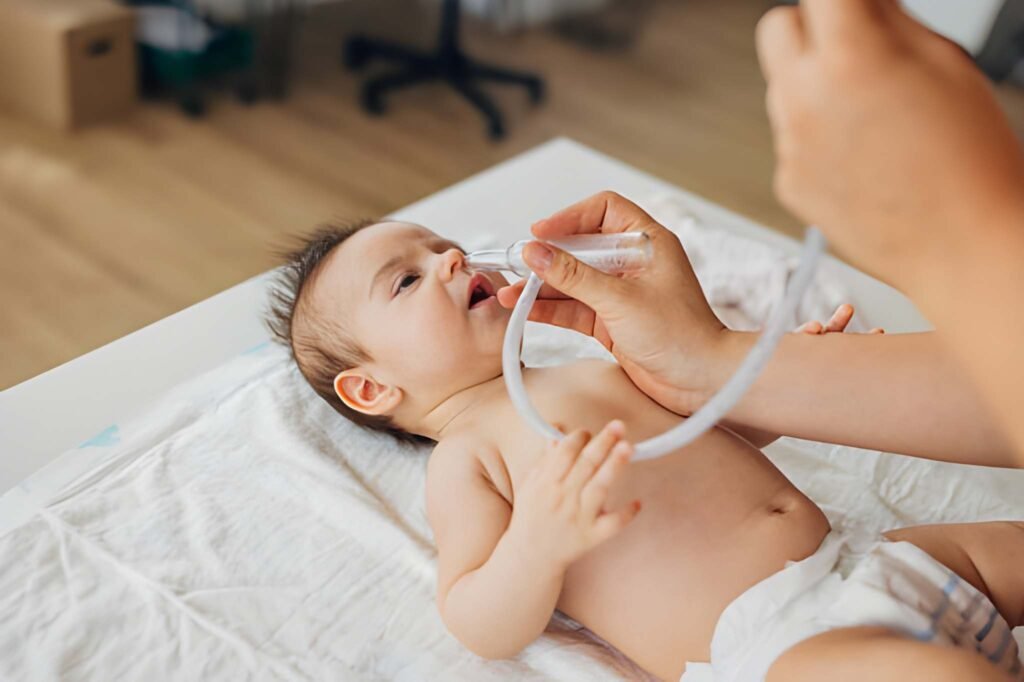
A newborn’s breathing often sounds surprising to first-time parents. From snorts and whistles to rhythmic congestion, the auditory landscape of a nursery is frequently dominated by nasal activity. Seeing a steady stream of clear mucus in a newborn’s nose is common, yet it often triggers concern. However, in the vast majority of cases, this drainage represents a healthy, functioning respiratory system adapting to the outside world. To manage this phase effectively, we must look at the biological reasons for mucus production and the specific tools designed to help infants breathe comfortably.
Why Newborns Produce So Much Mucus
The transition from the womb to the air-filled world is an immunological and physiological marathon. While in the womb, a fetus lives in a sterile, liquid environment. After birth, the respiratory tract must immediately begin filtering air, dust, and pathogens. Clear mucus serves as the first line of defense. It acts like a biological flypaper, trapping microscopic particles before they can reach the delicate lung tissue.
The Amniotic Clearing Process
In the first few days of life, clear mucus is often a remnant of amniotic fluid. During a vaginal birth, the "thoracic squeeze" of the birth canal helps expel much of this fluid from the lungs and upper airways. For babies born via Cesarean section, this squeeze does not occur, often leading to a few extra days of "wet" breathing as the body reabsorbs or expels the lingering fluid through the nose and mouth. This is a temporary developmental milestone, not a sign of illness.
The Unique Anatomy of Infant Airways
To understand why clear mucus causes so much noise, we must look at the scale of the newborn anatomy. A newborn's nasal passages are roughly the width of a drinking straw. Because these passages are so narrow, a tiny amount of swelling or a single drop of mucus can significantly narrow the airway. This creates the "whistling" or "rattling" sound parents hear during sleep or feeding.
Furthermore, newborns lack the muscle coordination and strength to blow their noses. While an adult can clear a nasal obstruction with a single forceful exhale, a newborn relies on sneezing—a primitive reflex—to move mucus forward. If the sneeze doesn't clear the path, the mucus remains in place, thickening as it is exposed to dry air.
Deciphering Clear vs. Colored Drainage
The color of nasal discharge provides important clues about what is happening inside the respiratory tract. For newborns, the consistency is often more telling than the color alone. Clear, thin mucus is typically a sign of normal clearing or a reaction to a mild environmental irritant.
| Mucus Color | Typical Meaning | Care Strategy |
|---|---|---|
| Clear & Thin | Normal clearing; mild irritants. | Saline and observation. |
| Clear & Sticky | Dehydration or dry air. | Increase humidity; check feeding. |
| White/Cloudy | Inflammation or early viral response. | Monitor for fever or lethargy. |
| Yellow/Green | Active immune response (not always infection). | Consult pediatrician if persistent. |
Environmental Irritants and Triggers
In the United States, modern household environments are often much dryer than a newborn's biological history prefers. Central heating and air conditioning systems strip moisture from the air, causing the delicate nasal mucosa to produce more mucus as a protective measure. This creates a paradoxical situation: dry air leads to "snotty" noses.
Common Household Triggers
Beyond dry air, several common household elements can trigger clear mucus production in a newborn:
- Pet Dander: Even if no allergy exists, the fine particles can irritate small airways.
- Strong Fragrances: Laundry detergents, perfumes, and scented candles can cause localized inflammation.
- Dust Mites: Soft surfaces like nursery rugs and stuffed animals are prime locations for dust accumulation.
- Temperature Fluctuations: Moving from a warm nursery to a cool outdoor environment causes the nasal vessels to constrict and then dilate, often resulting in a "runny" nose.
Management: Suction, Saline, and Steam
Managing clear mucus focuses on maintaining the "flow" of the drainage rather than stopping it. Stopping mucus production would leave the airway unprotected. Instead, we aim to thin the mucus and remove it gently when it interferes with feeding or sleep.
The Mathematics of Humidity Control
Pediatricians often recommend using a cool-mist humidifier to help with nasal clearing. The goal is to reach a relative humidity level of 40% to 50% in the nursery. If the air is too dry, the mucus hardens into "boogers" that can scratch the sensitive lining of the nose. If it is too humid (over 60%), you risk mold growth, which creates a new set of respiratory issues.
To move from 20% humidity (standard heated home) to 45% humidity:
A standard humidifier must evaporate approximately 0.5 to 0.75 gallons of water every 24 hours for a room of this size.
Safety Tip: Always use distilled water in humidifiers to prevent the dispersal of mineral dust, which can act as a nasal irritant.
When to Call the Pediatrician
While clear mucus is usually benign, it is vital to monitor how the baby is *coping* with the congestion. Because newborns are so small, respiratory distress can escalate quickly. In the US, pediatricians emphasize "Work of Breathing" as the primary metric for safety.
Nasal Flaring: The nostrils widen significantly with every breath as the baby tries to pull in more air.
Retractions: The skin pulls in around the ribs or at the base of the throat during inhalation. This looks like "tugging."
Grunting: A short, rhythmic sound at the end of each exhale. This is the baby's way of trying to keep their lungs open.
Cyanosis: A blue or dusky tint around the lips or fingernails. This is a medical emergency.
Yes. Because babies must breathe through their nose while sucking, a clogged nose can make feeding frustrating. If your baby is pulling off the breast or bottle frequently to gasp for air, use saline and suction 15 minutes before the next feed.
A Natural Transition
As we move through , the understanding of neonatal respiratory health continues to emphasize gentle intervention. Clear mucus is rarely an enemy; it is more often a shield. By maintaining a humid environment, using saline judiciously, and observing the baby's overall comfort, parents can navigate this "noisy" phase with confidence. Most babies outgrow this initial congestion as their nasal passages double in size over the first year. Until then, a little clear mucus is simply part of the developmental journey into a world full of new things to breathe.