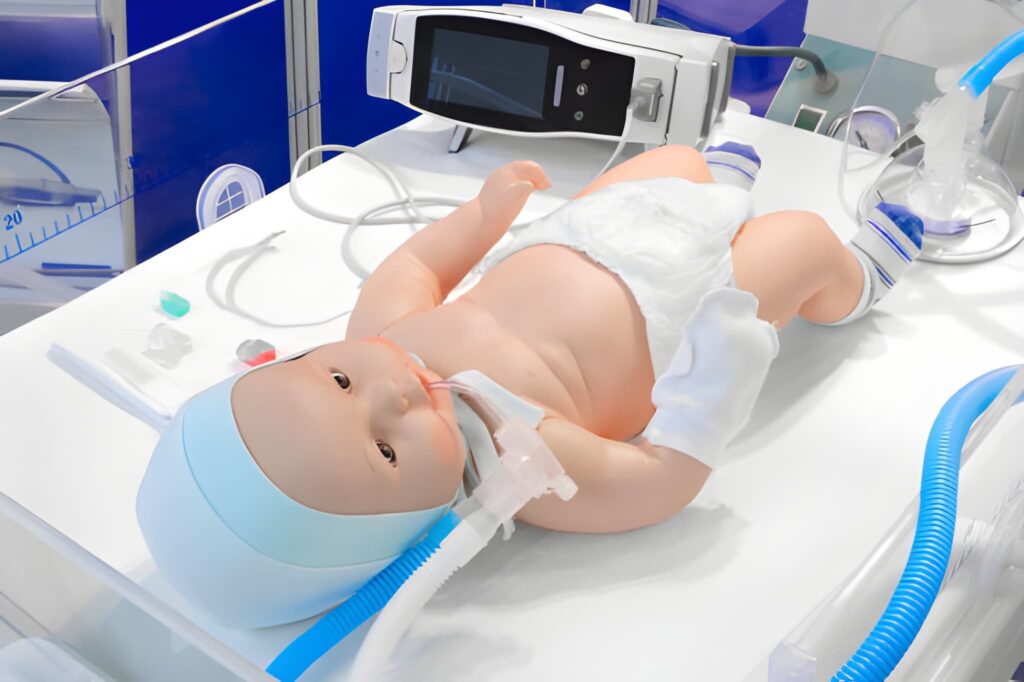
Newborn Respiratory Crisis: Immediate Clinical Management
The seconds following delivery constitute the most critical physiological transition in human life. A newborn must shift from receiving oxygen via the placenta to utilizing their own lungs to oxygenate their blood. When this transition fails, and an infant enters severe respiratory distress immediately after birth, the medical team must act with precision and speed. In , clinical protocols focus on the "Golden Hour"—the first sixty minutes of life—where rapid stabilization determines long-term neurological and pulmonary outcomes.
The Physiological Transition: Liquid to Air
In utero, the fetal lungs remain filled with fluid, and the pulmonary blood vessels are tightly constricted. This high resistance directs blood flow away from the lungs toward the placenta. At the moment of birth, three critical events must occur: the fluid must be cleared from the air sacs (alveoli), the lungs must expand with air, and the pulmonary blood vessels must dilate to allow blood flow.
The First Breath
The initial breath creates high negative pressure—often up to 70 cm H2O—to overcome the surface tension of the fluid-filled alveoli. This effort requires significant energy. If the surfactant system is immature or if the fluid clearance is delayed, the infant will struggle to maintain the functional residual capacity required for stable breathing.
Recognizing the Signs of Severe Distress
Respiratory distress in a newborn is rarely subtle. It manifests through a cluster of compensatory mechanisms where the infant attempts to maximize oxygen intake and prevent alveolar collapse. Understanding these signs is the first step in clinical triage.
- Central Cyanosis: A bluish tint to the tongue and trunk indicating low systemic oxygen.
- Expiratory Grunting: The infant exhales against a partially closed glottis to create backpressure and keep alveoli open.
- Nasal Flaring: An attempt to reduce airway resistance at the entry point.
- Retractions: Visible sinking of the skin around the ribs (intercostal), above the sternum (suprasternal), or below the ribs (subcostal) during inhalation.
- Tachypnea: A respiratory rate exceeding 60 breaths per minute.
Differential Diagnosis: Identifying the Cause
Severe distress immediately following delivery suggests a specific set of underlying conditions. The timing of the distress—specifically occurring at the moment of birth—narrows the diagnostic possibilities.
Primarily affects preterm infants due to surfactant deficiency. The lungs are stiff and collapse easily. On chest X-ray, this appears as a "ground glass" pattern with low lung volumes.
Often seen in term infants, especially those delivered via Cesarean section without labor. It results from delayed clearance of fetal lung fluid. While often milder, it can present severely in the first hour.
Occurs in term or post-term infants who have inhaled meconium-stained fluid. This causes mechanical obstruction, chemical inflammation, and surfactant inactivation.
Results from an infection acquired in utero or during the passage through the birth canal. Often associated with prolonged rupture of membranes or maternal fever.
Respiratory Scoring Systems
Objective measurement is essential for tracking an infant's progress or decline. While the Apgar score provides a general overview of transition, the Silverman-Anderson Score focuses specifically on the degree of respiratory distress.
A higher score indicates more severe distress. The score evaluates five areas:
- Upper chest synchronization
- Lower chest retractions
- Xiphoid retractions
- Nasal flaring
- Expiratory grunt
Immediate Stabilization: The Golden Hour Protocols
When a newborn is in severe distress, the medical team follows a tiered approach to stabilization, often referred to by the acronym S.T.A.B.L.E. (Sugar, Temperature, Airway, Blood pressure, Lab work, Emotional support).
The first intervention is often CPAP (Continuous Positive Airway Pressure). This provides a constant stream of air to keep the lungs inflated. If the infant's heart rate is low or breathing is gasping, Positive Pressure Ventilation (PPV) via a mask is initiated. In severe cases, intubation and mechanical ventilation are required immediately.
For preterm infants or those with severe MAS, synthetic surfactant is delivered directly into the lungs through an endotracheal tube. This rapidly reduces the surface tension and allows the lungs to expand with less effort.
A cold baby is a stressed baby. Hypothermia increases oxygen consumption and worsens metabolic acidosis. The infant must be placed under a radiant warmer or in a warmed isolette immediately during the stabilization process.
NICU Advanced Support and Diagnostics
Once the infant is stabilized, they are moved to the Neonatal Intensive Care Unit (NICU) for definitive diagnosis and long-term management. This phase involves high-tech monitoring and specialized imaging.
| Diagnostic Tool | Clinical Purpose | Standard Timing |
|---|---|---|
| Arterial Blood Gas (ABG) | Measures pH, pO2, and pCO2 to assess gas exchange and acidosis. | Within 30 minutes of distress. |
| Chest X-Ray | Visualizes lung expansion, fluid, or air leaks (pneumothorax). | Immediately following stabilization. |
| Echocardiogram | Evaluates heart structure and checks for pulmonary hypertension. | If distress persists despite support. |
| Blood Cultures | Identifies bacterial pathogens to guide antibiotic therapy. | Before the first dose of antibiotics. |
The US Healthcare Context: Access and Transport
In the United States, the management of severe neonatal respiratory distress is heavily influenced by the "Level of Care" system. Not all hospitals are equipped to handle an infant in severe crisis. Facilities range from Level I (Well Newborn Nursery) to Level IV (Regional NICU with surgical capabilities).
A critical component of US neonatal care is the Neonatal Transport Team. These highly specialized teams act as "mobile NICUs," capable of intubating, ventilating, and providing advanced medications like inhaled nitric oxide while moving a baby from a community hospital to a regional center. Access to these levels of care is a major determinant in survival rates. Socioeconomic factors, including insurance coverage and proximity to urban centers, can impact the speed with which a newborn receives this advanced life support. Federal programs like Medicaid provide a safety net, but the geographical "NICU deserts" remain a point of focus for maternal-child health advocacy.
The Specialist's Perspective on Recovery
While the sight of a newborn in respiratory distress is frightening for parents, modern neonatology provides an incredible success rate. Most infants who experience TTN or mild RDS recover within days. Even severe cases, when managed within the "Golden Hour" framework, often show remarkable resilience. The primary goal is neuroprotection—ensuring that the brain receives a steady supply of oxygen while the lungs heal. Through meticulous monitoring and family-centered care, we guide these fragile patients toward a healthy home discharge.