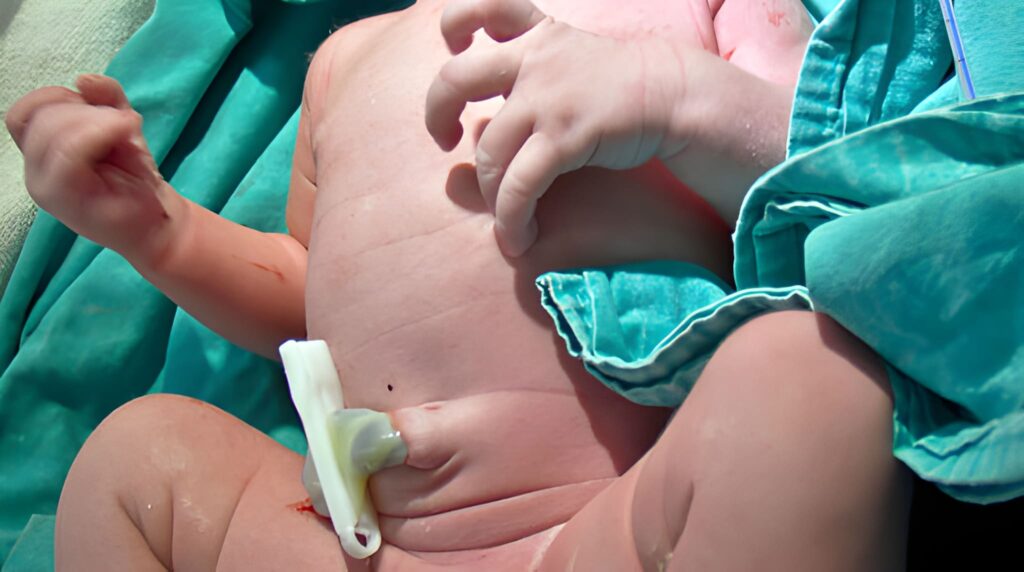
The Navel Journey: Managing Newborn Umbilical Bulges, Beads, and Bleeding
The transition from intrauterine life to the external world involves many physiological closures. Among the most visible is the healing of the umbilical cord. For many parents, the appearance of the newborn’s midsection—ranging from the drying stump to the shape of the emerging belly button—is a source of significant anxiety. When a parent notices a bulge when the baby cries or a persistent, red "bead" in the center of the navel, they are often witnessing common developmental milestones that require specific care rather than emergency intervention.
Lifecycle of the Umbilical Stump
At birth, the umbilical cord is a gelatinous, bluish-white structure containing two arteries and one vein. Once clamped, this tissue begins a process called dry gangrene—a normal, healthy process where the tissue dehydrates and eventually separates from the living tissue of the abdominal wall. Typically, the stump falls off within 7 to 21 days.
The cord transitions from white to yellow, then brown. It becomes hard and brittle. This is the stage where "dry care" is most critical to prevent bacterial colonization.
The base of the cord may appear slightly moist. A small amount of dark, dried blood or clear fluid is normal as the last attachments release.
Umbilical Hernias: The Protruding Bulge
Many parents report that their newborn’s stomach "bulges" or "pops out," particularly when the infant cries, coughs, or strains during a bowel movement. This is almost always an umbilical hernia. It occurs because the umbilical ring—the opening in the abdominal muscles through which the cord passed—has not yet fully closed.
Physiological Basis: During fetal development, the abdominal muscles grow toward the midline. If the fascia (connective tissue) does not fuse tightly after birth, a small gap remains. When intra-abdominal pressure increases, a small portion of the intestine or fatty tissue pushes through this gap, creating a visible bulge under the skin.
Umbilical Granulomas: The Persistent Bead
If the cord falls off but the center of the belly button remains moist and a small, pinkish-red "bead" of tissue is visible, it is likely an umbilical granuloma. This is an overgrowth of healing tissue (granulation tissue) that contains small blood vessels. It is not a scar, nor is it an infection; it is essentially the body trying "too hard" to heal the site.
A granuloma typically looks like a small, moist, red ball of flesh (the "bead") at the base of the navel. It may leak a small amount of straw-colored or slightly bloody fluid. Unlike an infection, a granuloma does not cause redness of the surrounding skin, fever, or pain for the infant.
Specialists often treat these with silver nitrate during a routine office visit. The silver nitrate "cauterizes" the excess tissue, causing it to turn black and eventually fall off. Another home-based treatment gaining clinical support involves the application of small amounts of common table salt to the bead, which dehydrates the tissue over several days.
Distinguishing Normal Oozing from Infection
Minor bleeding is the most frequent reason for pediatric calls regarding the umbilicus. It is helpful to categorize these events by their cause and volume.
| Symptom | Normal Presentation | Infection (Omphalitis) |
|---|---|---|
| Discharge | Clear, yellow, or slightly bloody; minimal volume. | Pus-like (cloudy/white), foul-smelling, or heavy volume. |
| Surrounding Skin | Matches the rest of the abdomen; no warmth. | Red streaks, spreading redness, or warm to the touch. |
| Infant Behavior | Unbothered by cleaning; feeding well. | Fussy, crying when navel is touched, or lethargic. |
| Bleeding | Spotting on the diaper or onesie (1-2 drops). | Active, continuous bleeding that recurs after pressure. |
Evidence-Based Daily Care Protocol
For decades, parents were told to use rubbing alcohol on the cord stump. Current medical consensus has shifted away from this practice. Research indicates that alcohol can kill the beneficial bacteria that help the cord separate naturally, actually delaying the process.
The "Clean and Dry" Strategy
Follow these steps to ensure optimal healing for your newborn’s navel:
- 1. Air Exposure: Fold the front of the diaper down so the cord is exposed to air. This promotes dehydration.
- 2. Sponge Baths Only: Avoid submerging the baby in a tub until the cord has fallen off and the site is dry.
- 3. Minimal Interference: If the cord becomes soiled with urine or stool, clean it gently with plain water and a cotton swab, then pat it thoroughly dry.
- 4. Let it Fall: Never pull or tug on the cord, even if it is hanging by a thread. Tension can cause unnecessary bleeding and irritation.
When Professional Intervention is Mandatory
While most umbilical issues are benign, certain presentations require an immediate call to the pediatrician or a visit to the pediatric emergency department.
A Summary of Concern Levels
Use the following breakdown to assess your newborn's situation today:
Bulge that goes away when the baby sleeps; cord that smells slightly "musty" without discharge; one drop of blood after the cord falls off.
The "bead" (granuloma) that hasn't healed after 3 weeks; persistent yellow oozing without skin redness; a hernia that seems to be getting significantly larger.
Fever over 100.4 F; redness spreading onto the abdominal skin; foul-smelling pus; a bulge that cannot be pushed back in.
As a specialist, I encourage parents to trust the "clean and dry" method and to observe the midsection with patience. The vast majority of umbilical hernias close on their own by age 3 or 4 without any surgical intervention, and granulomas are easily managed in a primary care setting. Your child's belly button is a lasting badge of their first connection to you—giving it time to heal naturally is the best care you can provide.